Heart Rate Recovery: What Your Number Means (And Why It Matters More Than You Think)

Key Takeaways
- A slow recovery doubles your risk of dying — and that finding has held up for 25 years. If your heart rate drops fewer than 12 beats in the first minute after exercise, multiple large studies link it to significantly higher mortality.
- It's a reflection of your underlying fitness, not a separate thing to fix. Improve your health, and the number follows.
- Six weeks of regular aerobic exercise can shift it. Heart rate recovery is one of the most modifiable mortality predictors — and the improvement starts sooner than you'd expect.
How quickly your heart rate drops after exercise tells you a lot about your health — and how long you're likely to live.
It's called heart rate recovery. And the research behind it is striking: if yours is slow, your risk of dying roughly doubles. That finding was first published in 1999. It's been confirmed repeatedly in the 25 years since, across hundreds of thousands of people.
Most smartwatches now track it. But the number they give you is harder to interpret than it looks — because what you do in the seconds after you stop exercising changes the reading significantly.
In this article, I'll walk you through what heart rate recovery actually is, what the science says about why it matters, what a good number looks like for your age, how to measure it properly, how to improve it, and my honest verdict on whether it's worth tracking.
I'm Dr. Eoghan Colgan. I've been a doctor in the NHS for nearly 25 years. Medical school taught me almost nothing about this, so I've been doing my own investigating.
What Is Heart Rate Recovery?
When you exercise, your muscles need more fuel and oxygen to produce energy — and they generate waste that needs clearing. So your heart speeds up to pump more blood — driven by your sympathetic nervous system, the same system that manages your fight-or-flight response. Think of it as your heart's accelerator pedal.
When you stop, your muscles no longer need the extra blood, so your heart slows back down. This is controlled by your parasympathetic nervous system — specifically the vagus nerve. Your heart's brake pedal.
In a healthy person, that brake is fast and strong. Your heart rate drops sharply in the first 60 seconds. But if you're deconditioned, or you have underlying health problems, the brake is sluggish. Your heart rate comes down slowly.
The speed of that drop — specifically, how many beats per minute your heart rate falls within one minute of stopping — is your heart rate recovery.
There are actually two phases. The first 60 seconds is driven almost entirely by your vagus nerve slamming the brakes on. After that, a slower phase takes over as adrenaline clears from your bloodstream and your sympathetic nervous system gradually stands down. That slower phase continues for five to ten minutes.
But it's the first minute that matters most. That's the measure the research focuses on, and the one most watches report.
I also cover this topic in a video on my YouTube channel - https://www.youtube.com/@stressfreelongevity
Why Does It Matter?
The landmark study was published in the New England Journal of Medicine in 1999. Researchers at the Cleveland Clinic followed over 2,400 adults — average age 57 — for six years. They measured heart rate recovery after a treadmill exercise test, with patients walking slowly as part of the cool-down.
If heart rate dropped by 12 beats per minute or fewer in that first minute, the risk of dying roughly doubled. After adjusting for age, fitness, medications, and the results of cardiac imaging, slow recovery remained an independent predictor of death.
That finding has been replicated many times. A 2017 meta-analysis pooling over 41,000 participants found that poor heart rate recovery was associated with a 68% higher risk of dying from any cause. A Mayo Clinic study of nearly 20,000 patients confirmed it predicted mortality across all age groups — from the 30s to the 70s — and in both men and women.
But here's the part that still surprises me.
A study of nearly 3,000 patients who had direct imaging of their coronary arteries found that heart rate recovery predicted death more strongly than the severity of the blockages themselves. How well your nervous system controls your heart matters as much — if not more — than how clear your arteries are.
The likely explanation is that heart rate recovery reflects something different from what a scan shows. It's measuring the health of your autonomic nervous system — the network that controls your heart rate, blood pressure, and dozens of other functions you never think about. When that system is impaired, the consequences go beyond any single artery.
This means heart rate recovery isn't something to fix in its own right. It's a reflection of your underlying health. You don't improve it by chasing a higher number. You improve the things it reflects — and the number follows.
Want the complete framework?
Get "The Vital 3 Method" free guide — 9 evidence-based principles across Sleep, Nutrition, and Exercise that improve your health whether you track heart rate recovery or not.
What Affects Your Number?
Before looking at what's normal for your age, it helps to understand what moves the number — because several of these factors change how you should interpret yours.
Fitness is the biggest modifiable factor. Regular exercisers have significantly faster heart rate recovery than sedentary people. One study of young adults found active individuals recovered nearly 50% faster than sedentary peers. The pattern holds across all ages — fitter people have stronger vagal brakes.
Age matters, but less than you'd expect. Heart rate recovery declines gradually with age, at roughly 2 beats per minute per decade. But the decline is non-linear. In healthy people without major risk factors, recovery stays remarkably stable from the 30s through the 50s — then drops more noticeably after 60. More on this shortly.
Medications change the reading. Beta-blockers — among the most commonly prescribed drugs for adults over 40 — actually make heart rate recovery look better. They blunt your peak heart rate, so the vagal brake appears to work faster against a lower ceiling. The number looks healthy even when underlying autonomic function may be impaired. If you're on a beta-blocker, your raw number is artificially inflated.
Tricyclic antidepressants and SNRIs raise resting heart rate through sympathetic activation, which would be expected to slow recovery. SSRIs appear to have no significant effect.
Diabetes impairs recovery even before symptoms appear. One study found diabetics without diagnosed nerve damage still had heart rate recovery 2–4 beats per minute lower than matched controls. The vagus nerve is one of the first things affected by the autonomic damage diabetes causes.
Obesity approximately triples the risk of an abnormal reading. Body fat percentage correlates strongly with slower recovery. Weight loss — beyond the benefit of the exercise used to achieve it — amplifies the improvement.
Body position makes an enormous difference. If you lie down immediately after exercise, your heart rate drops much faster than if you stay standing. Blood returns to your heart more easily when you're not fighting gravity — one study found heart rate was nearly 20 beats per minute lower in the lying position at the one-minute mark. This is why the threshold for "abnormal" depends entirely on what you did after stopping.
Day-to-day factors move the number too. Caffeine can delay parasympathetic reactivation. Poor sleep suppresses your parasympathetic system. Dehydration raises your working heart rate and slows recovery. A single reading on a bad day means very little.

Heart Rate Recovery by Age
With that context in mind, here are the reference ranges from the largest study to report age-specific data.
The Mayo Clinic study tracked nearly 20,000 adults and reported results for a "pure" cohort — healthy individuals free of hypertension, diabetes, smoking, and obesity. All measurements used 1-minute recovery with an active cool-down walk.
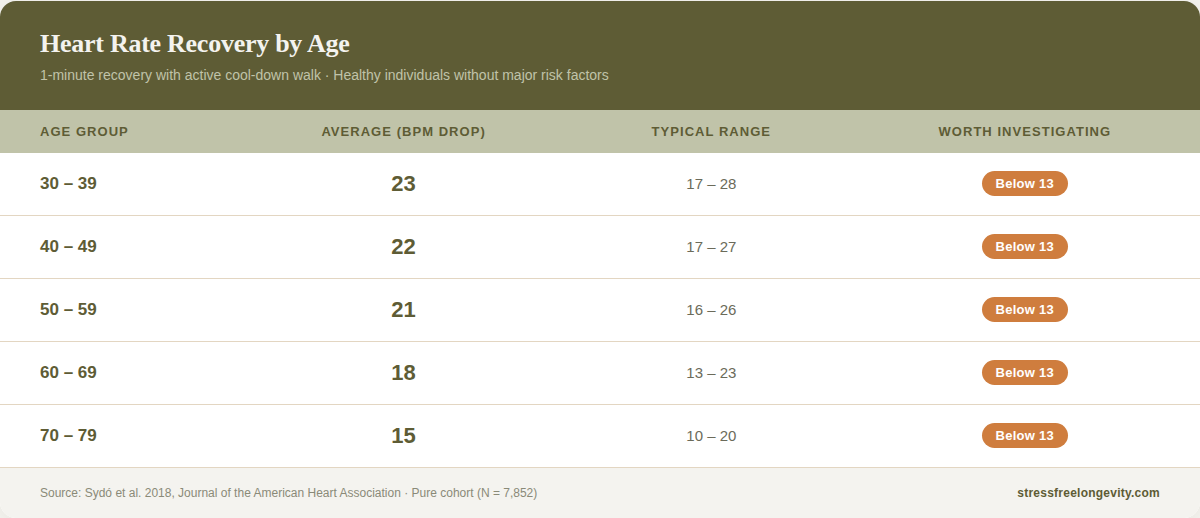
The ranges within each group are wide — that's partly fitness, partly genetics, and partly the inherent variability of the measurement.
But the most striking finding is how stable the number is from the 30s through the 50s. In healthy people, the median barely moves — 22, 22, 21. If you're 45 with a consistently low reading, you can't dismiss it as ageing. Your healthy peers have essentially the same recovery as 30-year-olds.
The decline accelerates after 60, which aligns with what we know about age-related changes in autonomic function. But even in the 70s, there's a wide range — and regular exercise keeps the number higher regardless of age.
One important note: these numbers come from a treadmill test with an active cool-down. If your watch measures recovery while you're standing still or sitting down, the thresholds are different. More on that in the next section.
How to Measure It Properly
This is where most of the confusion lives.
The threshold depends on the protocol.
The widely cited "12 beats per minute" threshold comes from the 1999 study, where patients walked slowly during recovery. That's an active cool-down. With an active cool-down, your heart rate stays slightly elevated from the movement, so a slower-looking recovery is expected. Below 12 indicates a problem.
If you stop and sit or lie down — a passive recovery — your heart rate drops faster. The equivalent abnormal threshold is higher, around 18 beats per minute at one minute.
Most people don't walk at a standardised pace after their workout. They stop, stand around, maybe sit down. So comparing your number to the 12-beat threshold from an active-recovery study isn't quite right.
Your smartwatch has a timing problem.
Heart rate recovery is the only one of the major fitness metrics that depends on when you press "end workout." Resting heart rate and HRV are measured overnight. VO2 max is estimated during the workout itself. But for heart rate recovery, your watch measures the drop from whatever your heart rate was when you stopped the timer.
If you forget to end your workout at peak effort and do it a few minutes later, your heart rate has already recovered. The number will look artificially low.
Apple Watch measures at 1 minute and 2 minutes after you end the workout. Garmin measures at 2 minutes. Both require you to end the workout at peak exertion for an accurate reading.
WHOOP doesn't measure heart rate recovery at all. Their "Recovery" score is a morning readiness metric based on overnight HRV, resting heart rate, and sleep — a different thing entirely.
A practical self-test protocol.
If you want a reliable reading you can track over time, standardise everything: use the same workout type each time, work hard enough that you're properly out of breath by the end, and end the workout immediately at peak effort.
Then either walk gently or sit down — but do the same thing every time. Check your heart rate exactly 60 seconds later. The difference between your peak and that 60-second number is your heart rate recovery.
If you walk, the standard concerning threshold is a drop of fewer than 12 beats. If you sit or lie down, your heart rate drops faster, so the equivalent threshold is around 18 beats.
Don't compare it to someone else's number. Don't compare it across different devices. Don't read too much into any single measurement — test-retest studies show that a single abnormal reading is confirmed on retest only about half the time. What you're looking for is a consistent trend over weeks and months.

How to Improve Yours
The most important thing about heart rate recovery is that it responds to the same interventions that improve everything else.
Aerobic exercise is the biggest lever. A large study of cardiac rehabilitation patients found that 41% of those with abnormal heart rate recovery normalised it within 12 weeks of regular exercise. And the patients who normalised had the same survival rates as those who were never abnormal. The number can change — and the change appears to matter.
Improvements can appear within six weeks. One study showed measurable shifts after just six weeks of training, three sessions per week. The earliest autonomic changes may begin around four weeks.
Intensity matters more than volume. Multiple studies have compared high-intensity interval training against steady-state moderate exercise for heart rate recovery. HIIT consistently wins — one trial found HIIT improved recovery by nearly 6 beats per minute at one minute, while moderate continuous training produced no significant change. For busy people, short intense sessions appear to deliver more than longer gentle ones.
That said, a foundation of regular moderate exercise — walking, cycling, swimming — still improves the number. The minimum effective dose appears to be around 75 minutes per week of moderate aerobic exercise.
Weight loss amplifies the effect. In one study, participants who lost more weight alongside their exercise programme gained over 6 beats per minute improvement, compared to less than 3 for those who exercised without significant weight loss.
Sleep and stress matter too. Your parasympathetic system — the brake — is suppressed when you're sleep-deprived or chronically stressed. Improving either will improve recovery. This connects directly to the other pillars: sleep quality and stress management aren't separate from cardiovascular fitness. They're part of the same system.
Gains reverse in about four weeks without training. One study found heart rate recovery returned completely to pre-training levels after four weeks of stopping. Consistency is the key variable. Two or three sessions per week, sustained over time, beats any short-term intensive block.
Should You Track It?
Honestly — it depends on what you'll do with the information.
Heart rate recovery reflects your underlying fitness and autonomic health. It doesn't add to it. If you're exercising regularly, sleeping well, and managing stress — your heart rate recovery is probably fine whether you look at it or not.
Where tracking has value is as a feedback tool. If you're making lifestyle changes and want to see them registering physiologically, a gently improving trend over months can be motivating. It's one more piece of the puzzle alongside resting heart rate, HRV, and VO2 max.
But the measurement is fiddly. You need to end your workout at the right moment, recover in the same position, and resist interpreting single readings. A bad night's sleep, a coffee before your workout, or forgetting to stop your watch at peak effort — any of these will throw the number off.
Personally, I track mine occasionally — it's useful as a trend, especially alongside my other metrics. Over the past ten months of gradually improving my fitness, it's trended upward. But I've also seen it drop when I forgot to stop my workout timer promptly, which is a good reminder that the number is only as good as the measurement.
Don't check it daily and don't overreact to a single reading. But if you notice a consistently low pattern over several weeks — that's worth paying attention to.

When It’s Worth Investigating Further
If you've been exercising regularly for 8–12 weeks and your heart rate recovery hasn't improved at all, it may be worth asking your doctor for a general check-up. You don't need to show them the metric — just mention that your fitness doesn't seem to be improving despite consistent effort. They can check for conditions that affect autonomic function: thyroid problems, diabetes, anaemia, or cardiovascular issues.
If low readings come alongside symptoms — unexplained fatigue, exercise intolerance, dizziness, or palpitations — that strengthens the case.
If you have diabetes, hypertension, or heart disease, your heart rate recovery may be lower for reasons related to your condition or medications. Track it if you find it useful, but discuss the readings with your doctor rather than interpreting them yourself.
The Bottom Line
Heart rate recovery is a genuine window into your cardiovascular and autonomic health. The science behind it is robust — 25 years of research, hundreds of thousands of participants, consistent findings.
But the number on your watch is only as useful as the measurement behind it. Standardise how you test, track trends over months, and don't lose sleep over a single reading.
The lifestyle is the thing that matters. Improve your fitness, and the number follows.

Ready to Improve What Actually Matters?
Heart rate recovery reflects your exercise, sleep, and stress levels. Get the foundations right and the number takes care of itself.
Get the complete Vital 3 Method guide — free:
- The 3 highest-impact changes for each pillar (9 total)
- The Build Good Habits framework to make them stick
- Start with one, build from there — no overhaul required
No spam. Unsubscribe anytime.
Frequently Asked Questions
Sources
- Cole CR et al. (1999). Heart-rate recovery immediately after exercise as a predictor of mortality. New England Journal of Medicine. PubMed
- Sydó N et al. (2018). Prognostic Performance of Heart Rate Recovery on an Exercise Test in a Primary Prevention Population. Journal of the American Heart Association. PubMed
- Qiu S et al. (2017). Heart rate recovery and risk of cardiovascular events and all-cause mortality. Journal of the American Heart Association. PubMed
- Nishime EO et al. (2003). Heart rate recovery after exercise is a predictor of mortality, independent of the angiographic severity of coronary disease. Journal of the American College of Cardiology. PubMed
- Villelabeitia-Jaureguizar K et al. (2017). Effect of high-intensity interval versus continuous exercise training on heart rate recovery in coronary heart disease. International Journal of Cardiology. PubMed
- Jouven X et al. (2005). Heart-rate profile during exercise as a predictor of sudden death. New England Journal of Medicine. PubMed
- Yawn BP et al. (2003). Concordance of heart rate recovery after exercise testing. Annals of Family Medicine. PubMed
Medical disclaimer
This content is for informational purposes only and is not intended as medical advice. Always consult your healthcare provider before making changes to your health routine. What works for one person may not work for another — this is a roadmap, not a prescription.
About Dr. Eoghan Colgan
Emergency medicine physician researching what actually works for longevity. I interview world-class experts in health and longevity and test everything personally. Everything I teach is what I'm implementing myself. More about me →

Related Articles
Types of Magnesium: What Actually Works (and What Doesn’t)
Types of Magnesium: What Actually Works (and What Doesn’t) Key Takeaways The form on the […]
GLP-1 Muscle Loss: What’s Real, What’s Overstated, and What to Do
GLP-1 Muscle Loss: What’s Real, What’s Overstated, and What to Do Key Takeaways The headline […]
How to Maintain Muscle After 40: What Actually Works
How to Maintain Muscle After 40: What Actually Works Key Takeaways Muscle loss after 40 […]



