How to Lower Blood Pressure Naturally: What Actually Works, Ranked by Evidence
Key Takeaways
- The most effective exercise for lowering blood pressure is a wall sit — not cardio. A 2023 meta-analysis of 270 trials found isometric exercise outperformed every other type of training.
- Realistic total reduction from lifestyle is 8 to 15 points, usually visible within 4 to 8 weeks. Enough to come off medication for some people, reduce the dose for others.
- Medication isn't failure. Some readings need lowering faster than lifestyle allows — and the two work better together than either alone.
If you've just seen a high blood pressure reading, you're probably wondering how much you can do about it without jumping to medication.
The short answer: quite a lot. Most people can lower their blood pressure by 8 to 15 points with lifestyle alone — enough to come off medication for some, reduce the dose for others, and meaningfully cut the risk of stroke, heart attack and dementia for everyone.
I'm Dr. Eoghan Colgan. I'm an emergency medicine physician, and I see what uncontrolled blood pressure does — the strokes, the heart failure, the kidneys that stopped working ten years before they should have. I've also seen patients put on medication when a few months of lifestyle changes would have been enough.
This article ranks the six lifestyle changes that have the biggest impact on blood pressure. Some are familiar — less salt, more movement, losing weight. One will definitely surprise you.
But first, we need to make sure the number you're trying to lower is even real.
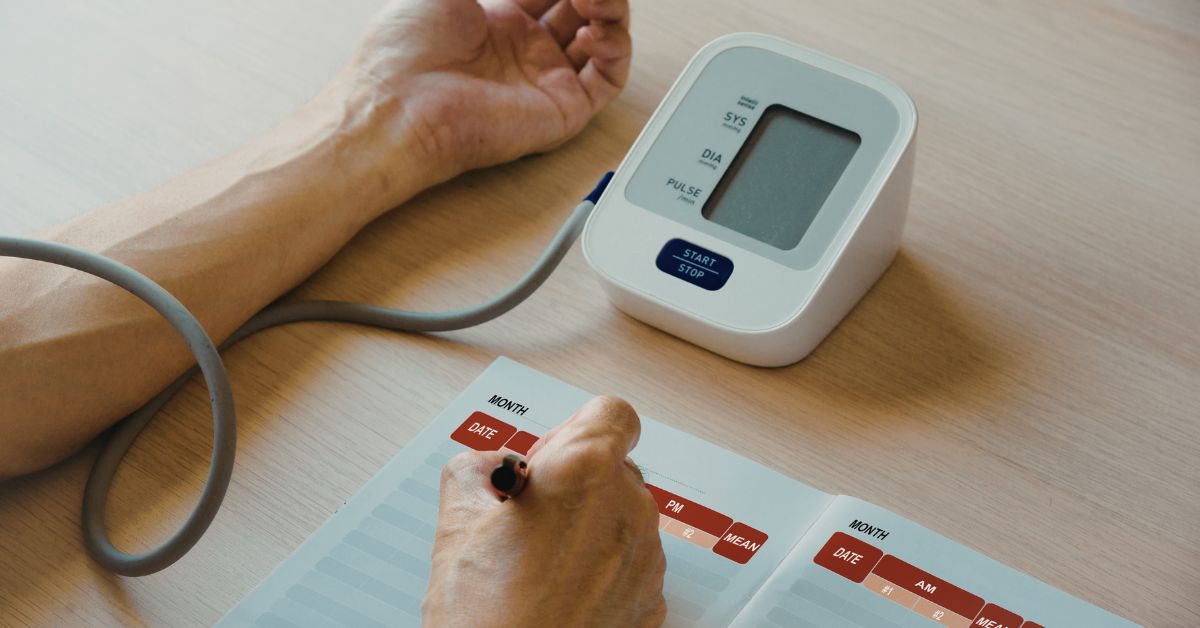
Is Your Reading Even Real?
Before you change anything, first check whether the number is accurate.
Blood pressure is one of the most variable measurements in medicine. It changes from second to second. A full bladder adds 10 points. Crossing your legs adds 8. Talking during the measurement adds up to 19. A cuff over a sleeve instead of bare skin can add 50.
The doctor's office is one of the worst places to measure it. Fifteen to 30 percent of people with high readings at the doctor have normal blood pressure at home — this is called white coat hypertension.
So measure it properly at home.
Buy a clinically validated upper-arm cuff. Most cost £20 to £40 ($30–50). Sit quietly for five minutes. Feet flat. Arm supported on a table in front of you with the cuff at heart level. No caffeine, smoking, or exercise in the preceding 30 minutes. Take three readings a minute apart — discard the first, average the next two. Do this morning and evening for a week.
If your home average is consistently over 130/80 you likely have hypertension and the rest of this article is for you. If it's lower than that, you probably don't — the reading at the doctor's was anxiety raising your number. Though you can still make positive lifestyle choices to avoid hypertension in the future.
So Your Reading Is High. What Now?
That depends on how high it is and whether you have symptoms.
If you have symptoms — phone the emergency services. A high reading (typically >180/100) combined with a severe headache, chest pain, sudden confusion, changes in vision, or difficulty speaking or moving is a medical emergency. Don't wait.
If your home readings are consistently 160/100 or higher but you feel well, see your doctor within the next few days. At this level, lifestyle changes alone take too long — the recommendation is to start medication alongside the lifestyle changes below. This isn't a failure. I'll cover it in detail later. Over time, with your doctor's guidance, you may be able to taper the dose or stop the medication once the lifestyle changes take effect.
If your home average is mildly elevated — say 130/80 to 159/99 — lifestyle changes alone are a reasonable first step. Most guidelines support a 3-to-6-month trial of lifestyle before starting medication, provided you don't have other major cardiovascular risk factors and your doctor agrees.
Either way — medication or not — the lifestyle changes matter. They lower blood pressure and improve the underlying health of your heart and arteries.
So here's what actually works.

The Six Lifestyle Changes With the Greatest Impact
Here are the six lifestyle changes with the strongest evidence, ranked by the size of reduction the research supports.
1. Wall Sits and Handgrip Holds (~7–8 points)
The most effective exercise for lowering blood pressure isn't cardio. It's a wall sit.
In 2023, researchers analysed 270 randomised trials involving nearly 16,000 people. They compared aerobic exercise, resistance training, HIIT, combined training, and isometric holds. Isometric produced the largest reduction: around 8 points systolic. That's roughly double what walking or jogging delivers, and comparable to a first-line blood pressure medication.
Isometric means holding a muscle under tension without moving. No reps, no running — just holding.
The two most tested forms are the wall sit and the handgrip squeeze. Both work the same way. When you hold that contraction, you temporarily squeeze the blood vessels inside the working muscles. The moment you release, blood rushes back in. Do this repeatedly over weeks, and your blood vessels become more elastic — better at expanding and contracting on demand. More elastic vessels handle blood with less pressure. Your resting number drops.
Here's how to do it.
Pick one — wall sits or a handgrip squeezer. Most people find wall sits easier to start with because you don't need any kit. A handgrip strengthener is useful if you have bad knees or want something you can do at your desk. It costs around £10 or $15.
For a wall sit: stand with your back flat against a wall, feet about two feet out from the wall, shoulder-width apart. Slide down until your thighs are roughly parallel to the floor — as if you're sitting in an invisible chair. Hold.
For a handgrip squeeze: grip the handle at about 30% of your maximum effort — firm but not straining. Hold. Switch hands between sets.
The protocol is the same for both: hold for two minutes, rest for two minutes, repeat four times. Three sessions a week. That's about 14 minutes a session.
If two minutes is too long at first, start at 30 seconds and build up. First results show at 2 to 4 weeks. Full effect by 8 to 12 weeks.
One important point: don't replace your other exercise with this. Walking, running, cycling, weights — they deliver benefits isometric exercise can't. Better fitness, stronger bones, sharper brain, better mood, longer life. Isometric is the most effective single type of exercise for lowering blood pressure. But for your overall health, you want the mix.

2. Eat Mostly Plants, Fish, and Whole Foods — and Cut Back on Salt (~7–11 points)
Changing how you eat is the biggest thing on this list. The catch is that it takes dozens of small choices, not one new habit.
The diet with the strongest evidence for lowering blood pressure is called DASH — Dietary Approaches to Stop Hypertension. It was developed in the 1990s specifically to bring blood pressure down. A landmark trial in the New England Journal of Medicine showed that people with high blood pressure who followed DASH and cut their salt intake lowered their systolic pressure by 11 points.
The diet is relatively straightforward.
Eat more of: Vegetables and fruit — aim for four to five servings of each per day. Whole grains — brown rice, oats, whole wheat bread. Fish, poultry, beans, nuts, and seeds. Low-fat dairy if you eat dairy.
Eat less of: Red and processed meat. Sugary drinks and sweets. Ultra-processed foods in general — packaged snacks, ready meals, fast food.
You don't need to follow a recipe plan or hit specific calorie targets. The closer you get to this pattern on most days, the more your blood pressure will drop.
Two nutrients inside this pattern do most of the work. You'll get more of one and less of the other just by eating this way — but they're worth understanding.
Cut the salt.
Sodium raises blood pressure by pulling water into your bloodstream. More water in your blood vessels means more pressure against the walls. Reducing salt reduces the volume, which reduces the pressure.
Most salt in the modern diet — around 70 to 75% — isn't from the salt shaker. It's hidden in bread, processed meats, cheese, sauces, soups, crisps, and restaurant food. Cooking at home more often is the single most effective way to cut your intake.
The practical target is under 2,300 mg a day — about one teaspoon of table salt. If you have high blood pressure, aim for under 1,500 mg. You'll get there by cooking at home more, reading labels, and eating out less.
Load up on potassium.
Potassium does the opposite of sodium. In the kidneys, it signals your body to flush excess sodium out in the urine, reducing blood volume. It also directly relaxes the walls of your blood vessels. A 2020 review found that increasing potassium intake lowered systolic blood pressure by around 4 points on its own.
Good sources: bananas, potatoes, sweet potatoes, beans, lentils, spinach, avocado, salmon, yogurt, and tomatoes. If you're eating the pattern above, you'll naturally hit the target range (3,500 to 5,000 mg a day) without tracking anything. Don't take potassium supplements without talking to your doctor first — they can cause problems if you have kidney issues or take certain blood pressure medications.
What to expect: The salt reduction shows up fast, within days to a couple of weeks. The full pattern takes about four weeks to reach peak effect. Together, they can lower systolic pressure by 7 to 11 points in someone with high blood pressure.
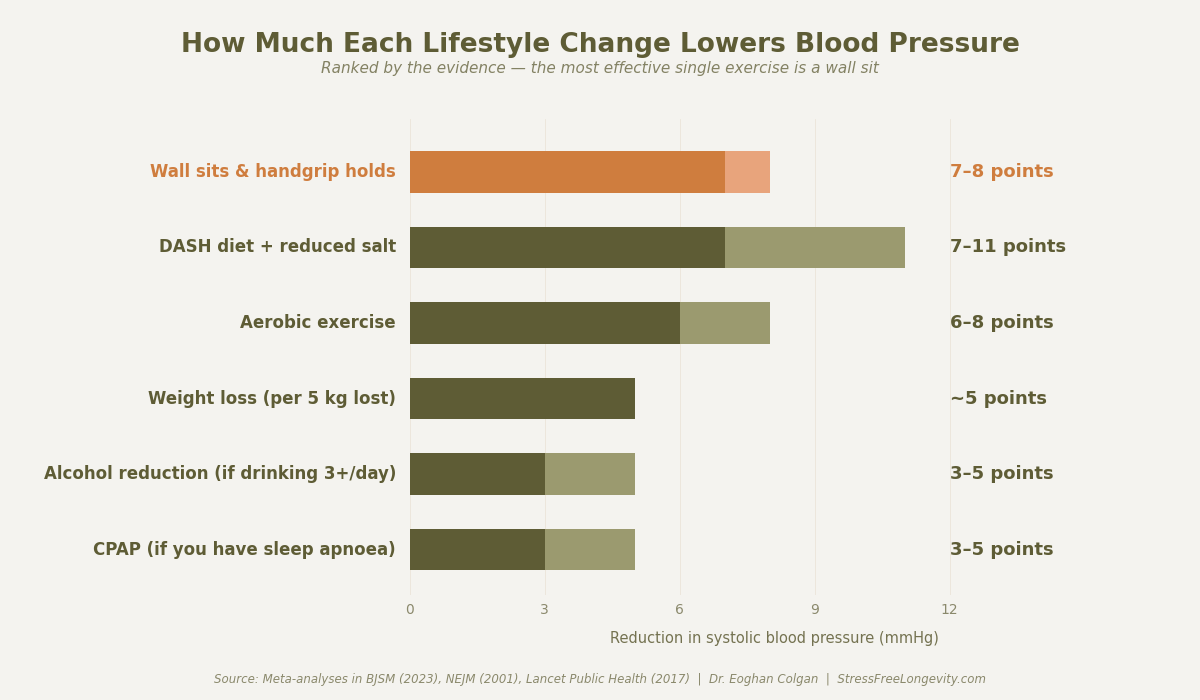
3. Move Regularly — Aerobic Exercise Plus Strength (~6–7 points)
Exercise is one of the most reliably effective things you can do for blood pressure — and for almost every other aspect of your health. The strongest evidence is for aerobic exercise. Adding strength training on top doesn't add much to the blood pressure effect, but it delivers other important benefits. You want both.
Aerobic exercise (the main driver).
Aerobic means anything that gets you breathing harder and your heart working — walking, running, cycling, swimming, dancing, climbing stairs. In people with high blood pressure, regular aerobic exercise lowers systolic pressure by 6 to 8 points.
It works in two ways. Over time, your heart becomes more efficient — it beats more slowly and pumps more forcefully at rest, which reduces the pressure it generates with each beat. Your blood vessels also become more flexible and responsive, so they accommodate the blood flowing through them with less resistance.
The target is 150 minutes a week of moderate aerobic exercise — meaning you're breathing harder than usual but can still hold a conversation. Brisk walking counts. Spread it across most days of the week — 20 to 30 minutes a day does it. If you're starting from a low base, five minutes of walking a day is better than nothing. Build from there.
Blood pressure starts dropping within 3 weeks, with the full effect by 8 to 12 weeks. One caveat: the benefit fades quickly if you stop. Consistency matters more than intensity.
Strength training (the supporting cast).
Strength training means working your muscles against resistance — weights, resistance bands, or bodyweight exercises like squats, lunges, press-ups, and rows.
On its own, strength training lowers systolic pressure by about 4 points — less than aerobic exercise. But it does things aerobic can't. It preserves muscle as you age, keeps your bones strong, improves glucose control, and protects against the kind of frailty that turns small falls into serious problems later in life.
Two or three sessions a week of 20 to 30 minutes covers it. Work your major muscle groups — legs, back, chest, shoulders, arms, core.

4. Lose Weight If You're Carrying Extra (~1 point per kg)
If you're carrying extra weight, losing some of it will lower your blood pressure — reliably, measurably, and fairly quickly.
The rule of thumb is about 1 point of systolic reduction per kilogram (2.2 pounds) lost. So a 5 kg loss gets you around 5 points. A 10 kg loss, around 10 points.
Two things to know. The rule holds up best in the first 6 months. Over 2 or 3 years, some of the benefit fades — partly because weight often creeps back, partly because the body adjusts. And the rule only applies if you're genuinely carrying extra weight. If you're already at a healthy weight, losing more won't lower your blood pressure.
How it works.
Extra weight — particularly around the abdomen — makes your body work harder in several ways. Your heart pumps harder to supply a larger body. The fat itself releases inflammatory signals that stiffen blood vessels. Excess weight drives insulin resistance, which promotes sodium retention. And it raises the risk of sleep apnoea, which independently raises blood pressure. Losing weight reverses each of these.
What to aim for.
You don't need to hit an "ideal" weight. The evidence shows meaningful blood pressure benefits from losing 5 to 10% of your starting weight. For someone at 90 kg, that's 4.5 to 9 kg. Sustainable loss of about half a kilogram (one pound) a week is a reasonable target.
The best weight loss approach is the one you can stick to. For most people, that means eating a bit less, combined with the eating pattern from #2 — plenty of plants, fish, and whole foods, with less processed food. Exercise helps, but changes to what you eat usually do the heavier lifting.
What to expect.
Blood pressure drops alongside the weight — you'll see it move within weeks of consistent loss. Full effect at 3 to 6 months. If the weight comes back, so does the blood pressure. Keeping it off matters.
5. Drink Less Alcohol — If You're Drinking More Than Two a Day (~3–5 points)
The more you drink, and the more you cut back, the bigger the benefit.
How it works.
Alcohol raises blood pressure through several mechanisms at once. It activates the nervous system signals that constrict blood vessels. It interferes with the hormones that control fluid balance. And heavy drinking damages the cells that line your blood vessels, making them stiffer and less responsive. The more you drink — and the longer you've been drinking at that level — the bigger the effect.
What to do.
If you drink more than two a day, cutting back is one of the highest-value things on this list. You don't have to stop entirely — halving your intake will move the number meaningfully. Many people find it easier to have several alcohol-free days a week than to cut down every evening.
If you already drink less than two a day, cutting further won't meaningfully lower your blood pressure. But alcohol does carry other health costs — cancer risk, disrupted sleep, weight gain — so drinking less is still worthwhile for other reasons. Just don't expect it to move your blood pressure number.
What to expect.
The effect shows up fast — within days to a couple of weeks.
6. Screen for Sleep Apnoea (~3–5 points if you have it)
This one's a little different. It only applies if you have a specific condition — obstructive sleep apnoea, or OSA — but if you do, treating it is one of the most effective things you can do for your blood pressure.
Sleep apnoea is where your airway partially or fully collapses during sleep, repeatedly cutting off your breathing for seconds at a time. Each time this happens, your body floods with stress hormones to restart breathing. Your blood pressure spikes. Your sleep fragments. This happens dozens — sometimes hundreds — of times a night, and most people have no idea it's happening. It's also one of the most common causes of difficult-to-treat hypertension in adults.
The signs to watch for:
Loud snoring, especially with pauses in breathing. Waking up with a dry mouth or headache. Feeling unrefreshed after a full night's sleep. Daytime sleepiness even when you've slept eight hours. A thick neck (17 inches or more in men, 16 inches or more in women) or a body mass index over 30.
If your partner has told you that you stop breathing at night, or if you tick several of these boxes, ask your doctor about a sleep study. Many can now be done at home with a small device you wear overnight.
Why it matters for blood pressure:
Treating sleep apnoea — usually with a CPAP machine, which keeps the airway open overnight — lowers systolic pressure by around 2 to 3 points on average, and up to 5 points in people with hard-to-control hypertension. Beyond the number, treated sleep apnoea also improves daytime energy, mood, and cognitive function, and independently reduces the risk of stroke, heart attack, and atrial fibrillation.
If sleep apnoea isn't the issue — what about general sleep?
The evidence that improving sleep quantity or quality lowers blood pressure in people without sleep apnoea is weaker than you'd expect. That doesn't mean sleep doesn't matter — poor sleep raises stress hormones, worsens weight control, and makes every other lifestyle change harder. Aim for 7 to 8 hours a night. Just don't expect it to move your blood pressure number much on its own.
Want the complete framework?
Get "The Vital 3 Method" free guide — 9 evidence-based principles across Sleep, Nutrition, and Exercise that improve your health and your blood pressure.
Do These Stack? Yes — But Not Simply
When you combine multiple lifestyle changes, you get a bigger drop than any single one delivers on its own. But the effects don't simply add up.
Several of the six work on the same things — how flexible your blood vessels are, how active your nervous system is, how much fluid is in your bloodstream. So when you combine them, each one has a bit less work left to do. Doing three changes doesn't give you three times the benefit. But it does give you more than any one change alone.
What the evidence shows.
Large trials combining multiple interventions consistently show around 10 to 15 points of systolic reduction in motivated people over 3 to 6 months. The landmark ENCORE trial, which combined the DASH diet with regular exercise and weight loss, saw systolic pressure drop by 16 points in people with stage 1 hypertension over four months. That's a bigger reduction than many blood pressure medications deliver.
Two caveats. People in those trials were supervised and motivated — real life is messier. A realistic sustained reduction for someone doing this on their own is 8 to 12 points. And you have to keep doing them, or the pressure creeps back up within weeks to months.
Where to start.
Don't try to do all six at once. You'll burn out within three weeks and give up. Start with one, build it into a real habit over 2 to 4 weeks, then add the next.
This order works well for most people:
Weeks 1–3: Start the wall sits or handgrip holds (#1). Fourteen minutes, three times a week. Low commitment, high return.
Weeks 3–6: Shift toward the DASH pattern and cut the salt (#2). Cook at home more. Add more vegetables, fruit, and whole foods.
Weeks 6–10: Build in regular aerobic exercise (#3). Walking is enough. Aim for 30 minutes most days.
Throughout: If you drink more than two a day, cut back (#5). If you're carrying extra weight, the DASH and exercise changes will start delivering the weight loss (#4) on their own. If you have any signs of sleep apnoea, raise it with your doctor (#6).
Make each change real before adding the next. A habit you'll keep beats a protocol you'll abandon.

The Medication Question
If your doctor recommends blood pressure medication, take it. It's not a failure. It's a tool, and a highly effective one.
Medication can lower your systolic pressure by 10 to 15 points. That's comparable to doing all six lifestyle changes perfectly. And every 10-point reduction cuts your risk of stroke by about 27%, heart failure by 28%, and dying early by 13%.
When medication should come first.
If your readings are consistently 160/100 or higher, or you have conditions like diabetes, heart disease, or kidney problems, your doctor will likely recommend starting medication straight away. At those levels, lifestyle changes alone take too long, and the longer your pressure stays high, the more damage accumulates. Start the medication and start the lifestyle changes alongside it.
Why you still need the lifestyle changes.
Medication lowers the number. It doesn't fix insulin resistance, inflammation, stiff blood vessels, or sleep apnoea. Lifestyle changes do. That's why people who do both get better results — lower blood pressure, fewer side effects, lower long-term cardiovascular risk — than medication alone delivers.
Coming off medication later.
Starting medication isn't a life sentence. In the landmark TONE trial, around 40% of older adults on blood pressure medication successfully came off it after combining weight loss and salt reduction, compared to 16% who didn't make those changes.
Once the lifestyle changes take hold, many people can reduce or stop their medication — always with their doctor's guidance. Never stop or reduce blood pressure medication on your own.
The bottom line.
Medication and lifestyle aren't opposing approaches. They're two parts of the same treatment. If your numbers are borderline and your risk is low, lifestyle alone for 3 to 6 months is reasonable. If your numbers are higher or your risk is significant, medication plus lifestyle is the safer, faster route.
Either way, the lifestyle changes matter.
What About Stress, Supplements, and the Rest?
There's a long list of things that come up in conversations about lowering blood pressure — herbs, supplements, specific foods, stress techniques. Here's an honest verdict on the most common.
Stress management, meditation, and slow breathing.
Structured practices like yoga, transcendental meditation, or regular slow-breathing exercises can lower systolic pressure by around 3 to 5 points in people with high blood pressure. The key word is structured — doing it regularly, for weeks, not occasionally. Meditation apps and breathing gadgets show weaker and less consistent effects. Worth doing for the broader benefits to mood and sleep, but don't expect dramatic BP changes.
Specific foods.
Beetroot juice, dark chocolate, hibiscus tea, and garlic all have real but modest effects. Beetroot delivers around 4 points of systolic reduction thanks to its nitrate content. Dark chocolate and hibiscus tea each deliver around 3 to 4 points in people with high blood pressure. These are real, but they're additions to a good diet — not replacements for it.
Supplements.
- Potassium — already covered in #2. The strongest supplement-like evidence, best obtained through food.
- Magnesium — around 2 points of reduction on average, bigger if you're deficient. Worth ensuring adequate intake through food (leafy greens, nuts, whole grains) before reaching for supplements.
- Omega-3 / fish oil — 2 to 4 points of reduction at high doses (2–3 g of EPA + DHA daily), less at normal doses.
- CoQ10 — older studies suggested large effects. Newer, better-designed studies show 3 to 5 points at most.
- Vitamin D — does not lower blood pressure. Take it for bone health if you're deficient, not for BP.
Caffeine.
A cup of coffee raises your blood pressure acutely — by about 5 to 8 points for a couple of hours. But regular coffee drinkers develop tolerance, and the long-term effect on resting blood pressure is negligible. If you drink coffee regularly, you don't need to quit for blood pressure reasons.
Smoking.
Here's a surprise: smoking doesn't reliably raise your resting blood pressure. The damage it does to your heart and blood vessels is enormous — but the direct effect on the number is small. Quit for every other reason, not for blood pressure.
A Note for Women in Perimenopause and Beyond
Blood pressure often rises during perimenopause and the years after menopause, even in women who previously had no issues. The drop in oestrogen reduces the natural flexibility of your blood vessels, and you become more sensitive to salt. It's a real physiological shift, not something you're imagining.
Everything in this article still applies — the six interventions work for women as well as men. But readings can change more quickly during this period, so it's worth measuring at home more often and raising any upward trend with your doctor. Hormone replacement therapy isn't a blood pressure treatment, but some women find their readings stabilise when HRT is part of their care. Discuss it with your doctor if you're already on HRT or considering it.

What If Nothing Works?
If you've done the lifestyle changes consistently for 3 to 6 months and your blood pressure hasn't moved much, something else may be driving it.
In 5 to 10% of cases, high blood pressure has an identifiable cause that lifestyle alone won't fix. This is called secondary hypertension. The common causes include:
- Sleep apnoea — covered in #6, but worth raising again here because it's the most common hidden driver
- Kidney problems — chronic kidney disease or narrowing of the arteries to the kidneys
- Primary aldosteronism — a hormonal condition where the adrenal glands produce too much of a hormone that raises blood pressure. Under-diagnosed, and worth testing for if you have hard-to-control hypertension
- Thyroid problems — both overactive and underactive thyroid can affect blood pressure
- Certain medications and substances — NSAIDs (ibuprofen, naproxen), decongestants, combined oral contraceptives, some antidepressants, licorice, and stimulants can all raise blood pressure
If your readings haven't responded to consistent lifestyle changes, or if they've suddenly risen with no clear reason, ask your doctor about investigating a secondary cause. A few simple blood and urine tests can rule out most of the common ones. This is worth pursuing — treating a secondary cause can normalise blood pressure completely.
The Bottom Line
Blood pressure responds to what you do.
Start with wall sits. Add the DASH diet. Build in regular exercise. Cut back if you drink more than two a day, lose weight if you're carrying extra, and get checked for sleep apnoea if you snore and wake tired.
Do these consistently and your systolic pressure drops by 8 to 15 points. Enough to come off medication for some people, reduce the dose for others, and cut the risk of stroke, heart attack, and dementia for everyone.
A small change you'll keep beats a big one you'll abandon. Start with one. Build it. Add the next.
And if your doctor recommends medication, take it. It's not a failure. It's a tool that works — and it works better alongside the lifestyle changes, not instead of them.

The Hard Part Isn't Knowing What to Do - It's making it stick.
You now have the six changes that lower blood pressure. The Vital 3 Method is the full system I used to lose 14kg, reverse my metabolic age, and bring my own numbers into a healthy range — without intensive protocols.
- The 3 highest-impact changes for each life pillar (9 total)
- The Build Good Habits framework to make them stick
- Start with one, build from there — no overhaul required
No spam. Unsubscribe anytime.
Frequently Asked Questions
Sources
- Edwards JJ et al. (2023). Exercise training and resting blood pressure: a large-scale pairwise and network meta-analysis of randomised controlled trials. British Journal of Sports Medicine. PubMed
- Sacks FM et al. (2001). Effects on blood pressure of reduced dietary sodium and the DASH diet. New England Journal of Medicine. PubMed
- Neter JE et al. (2003). Influence of weight reduction on blood pressure: a meta-analysis of randomized controlled trials. Hypertension. PubMed
- Roerecke M et al. (2017). The effect of a reduction in alcohol consumption on blood pressure. Lancet Public Health. PubMed
- Ettehad D et al. (2016). Blood pressure lowering for prevention of cardiovascular disease and death: a systematic review and meta-analysis. Lancet. PubMed
Medical disclaimer
This content is for informational purposes only and is not intended as medical advice. Always consult your healthcare provider before making changes to your health routine. What works for one person may not work for another — this is a roadmap, not a prescription.
About Dr. Eoghan Colgan
Emergency medicine physician researching what actually works for longevity. I interview world-class experts in health and longevity and test everything personally. Everything I teach is what I'm implementing myself. More about me →

Related Articles
Heart Rate vs VO2 Max vs HRV: Which Is the Most Useful?
Heart Rate vs VO2 Max vs HRV: Which Is the Most Useful? Key Takeaways VO2 […]
Heart Rate Recovery: What Your Number Means (And Why It Matters More Than You Think)
Heart Rate Recovery: What Your Number Means (And Why It Matters More Than You Think) […]
Is Sitting All Day Bad for You? (Yes — Even If You Exercise)
Is Sitting All Day Bad for You? (Yes – Even If You Exercise) Key Takeaways […]



