What Is a Good HRV? (And How to Improve Yours)

Key Takeaways
- Your trend matters more than today's number. A single HRV reading can swing 10-15% day to day. Your 7-day average is what tells the real story.
- Different devices measure different things. Apple Watch reports a different metric to Oura and WHOOP. You can't compare numbers across devices.
- Slow breathing has the strongest evidence for improving HRV. A meta-analysis of 223 studies confirms it. Five minutes a day, six breaths per minute.
If you've checked your HRV and want to know whether it's good, bad, or normal — you're in the right place.
The short answer: it depends on your age, your genetics, your device, and what happened in the last 24 hours. There's no single number that means "healthy."
But there are useful reference ranges. And there are patterns worth paying attention to.
In this article, I'll give you the numbers by age so you can see where yours sits. But I also want to walk you through the things that affect your HRV — some of them surprising — so you can actually make sense of what your watch is telling you. Including when a low number matters, when it doesn't, and what the evidence says about improving it.
First, a quick primer on what HRV actually is.
What Is HRV?
Your heart doesn't beat like a metronome. Even at a steady 60 beats per minute, the gap between beats varies — one might be 0.95 seconds, the next 1.05. That variation is your heart rate variability.
Two things control it. The first is your autonomic nervous system — the part running in the background without you thinking about it. Two branches pull in opposite directions: one speeds your heart up (the stress response), the other slows it down (the recovery response). The variation in your heartbeat reflects how well these two systems are balancing each other.
The second is the heart itself. Your heart's pacemaker cells have their own rhythm, and that rhythm contributes to variability too. So HRV isn't purely a nervous system measure — it's a window into both your autonomic health and your heart health.
More variation generally means a more adaptable system. Less variation can mean your body is under strain — from stress, poor sleep, illness, or ageing.
Research consistently links low HRV to poorer health outcomes — cardiovascular disease, higher mortality risk, greater vulnerability to stress. But this is where most articles get it wrong. Low HRV doesn't cause these problems. It reflects them. Your HRV is a window into your underlying health — when your sleep, fitness, stress levels, and metabolic health are in good shape, HRV tends to be higher. When they're not, it drops.
This means you don't improve your health by chasing a higher number. You improve the things that matter — and the number follows.

What Affects Your Number?
Before looking at the age-based ranges, it helps to know what moves the number — because several of these will change how you interpret yours.
Genetics account for roughly half your baseline. Twin studies suggest 47-74% of resting HRV is genetically determined. Some people are simply wired higher or lower. This is one reason comparing your number to someone else's is mostly noise.
Age is the next biggest factor. HRV drops steadily from your 20s onward, most steeply between 20 and 40, then gradually levelling off. This is normal — it reflects natural changes in your nervous system and blood vessels as you age.
Your device matters more than you'd expect. Most wearables — Oura, WHOOP, Garmin, Fitbit — report RMSSD, which captures your recovery system specifically. Apple Watch reports SDNN, a broader measure of total variability. These are fundamentally different metrics. An RMSSD of 40 and an SDNN of 40 are not the same thing. A 2025 validation study found Oura was within about 6% of medical-grade ECG, WHOOP within 8%, and Garmin within 10%. A separate study found Apple Watch had roughly 29% error — though this partly reflects its passive measurement approach.
Medications shift the baseline. Beta-blockers increase HRV by blocking the stress response — if you're on one, your number will look higher than it would otherwise. Some antidepressants work in the other direction, with tricyclics having the strongest lowering effect and SSRIs the mildest.
Alcohol suppresses HRV in a dose-dependent way. Two standard drinks reduce it by roughly 28-33%. One drink has no significant effect. Recovery depends on how much — a couple of drinks and you'll bounce back next day; a heavy night can suppress it for several days.
Hormones play a role. Before menopause, women tend to have slightly higher HRV than men of the same age. After menopause, this difference disappears — likely driven by oestrogen's effect on the autonomic nervous system.
Daily swings of 10-15% are completely normal. A bad night's sleep, a stressful day, a hard workout — any of these will move your number. That's your nervous system responding. It's not a problem.
Want the complete framework?
Get "The Vital 3 Method" free guide — 9 evidence-based principles across Sleep, Nutrition, and Exercise that improve your health whether you track HRV or not.
HRV by Age
With that context in mind, here are the reference ranges. The first is. based on RMSSD — the metric most wearables report.
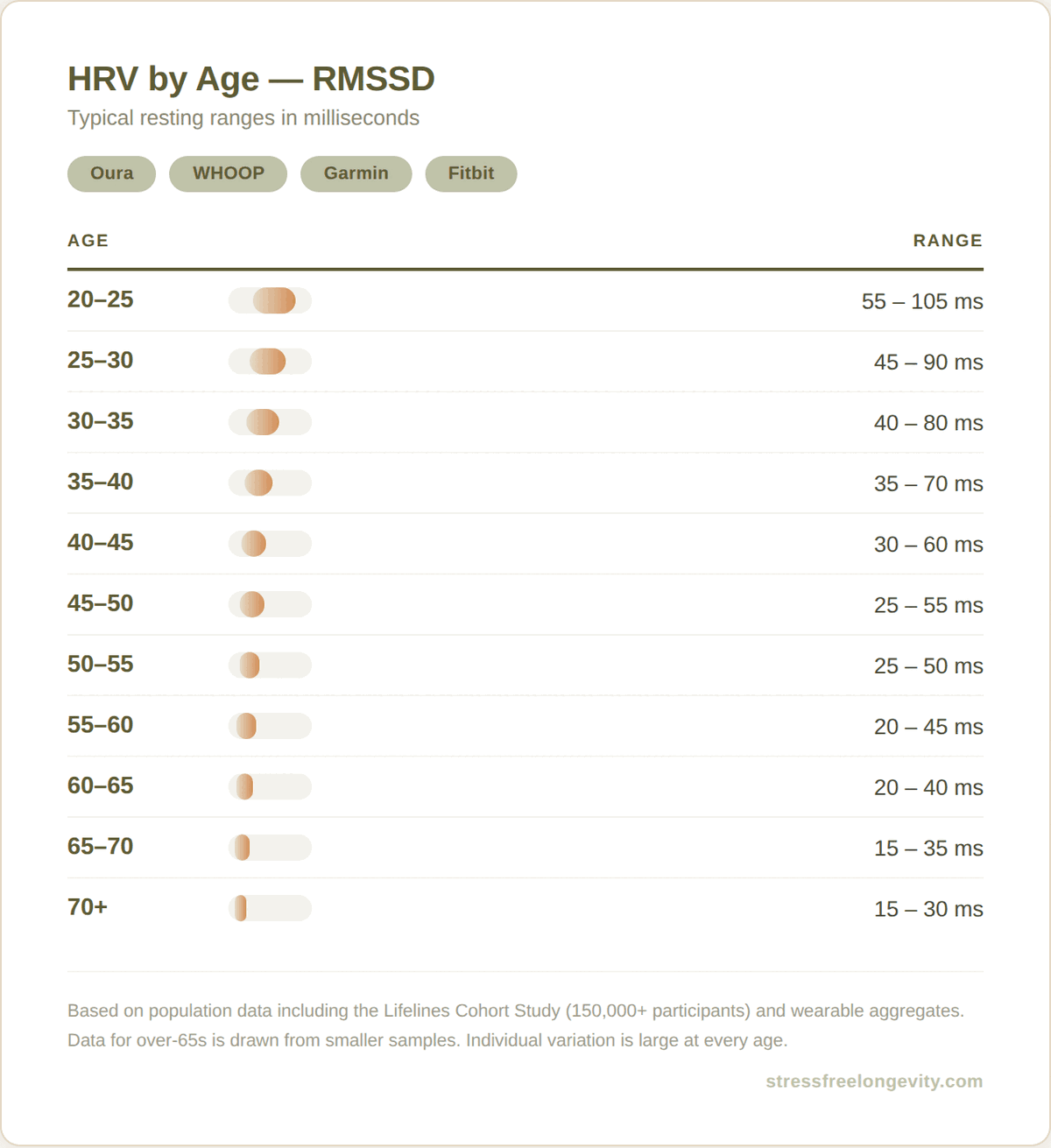
If you use Apple Watch, your device reports SDNN rather than RMSSD. These are different metrics and the numbers aren't interchangeable. Typical Apple Watch SDNN values are roughly:

A 2024 validation study found Apple Watch had roughly 29% measurement error compared to a chest strap. This is partly because Apple Watch measures passively at irregular intervals rather than during a controlled sleep window like Oura or WHOOP. Your trend is still informative — but the individual readings are less precise.
You'll notice the ranges within each age group are wide. That's partly genetics, partly lifestyle, and partly because HRV is one of the most variable health metrics there is — it can shift 10-15% from one day to the next based on sleep, stress, and what you did last night.
This is why individual readings aren't particularly helpful. What matters more is your trend. A stable HRV — or one that's gently improving alongside positive lifestyle changes — is a better signal than any single number. As HRV researcher Marco Altini has noted, comparing your HRV to your own averages over time tells you far more than comparing it to a chart.
So what are those positive lifestyle changes that actually shift the trend?
How to Improve Your HRV
Here's what the evidence actually supports, ranked by strength of research.
Slow breathing
A meta-analysis of 223 studies found that breathing at around six breaths per minute consistently increases HRV. It works by directly stimulating the vagus nerve — the main nerve of your recovery system. Five minutes a day is enough. You don't need an app, though one can help you keep the pace.
The effect occurs while you're doing it — but the lasting benefit comes from consistent practice over weeks.
Aerobic exercise
A meta-analysis of 16 randomised controlled trials found regular aerobic exercise significantly improves HRV. First measurable changes appear around four weeks, with meaningful shifts at eight to twelve weeks. Cross-sectional studies consistently show regular exercisers have higher HRV than sedentary peers of the same age. The type matters less than the consistency — walking, cycling, swimming. Just get a little out of breath, regularly. Explore my exercise content for more on getting started.
Reduce alcohol
Two standard drinks reduce HRV by roughly 28-33% acutely. Heavy drinking can suppress your baseline for several days. Chronic heavy drinking lowers resting HRV — and recovery takes months of abstinence, not days.
Sleep
Each additional hour of sleep adds measurably to overnight HRV. A bad night drops it; recovery typically takes one to two nights. If your HRV is consistently low and you're sleeping less than seven hours, start here.
Weight loss
Excess weight puts chronic strain on your cardiovascular and autonomic systems. One study in overweight adults with type 2 diabetes found that losing 10% of body weight increased RMSSD by 39%. Multiple systematic reviews confirm the pattern — losing weight reliably improves HRV.
A note on meditation
Mindfulness meditation alone doesn't reliably improve resting HRV — a meta-analysis of 19 randomised trials found no significant effect. Where meditation does seem to help is when it includes a slow breathing component. If your practice already involves focused breathing, you're likely getting the benefit. If it doesn't, consider adding it.

Should You Track Your HRV?
Honestly — it depends on what you'll do with it.
HRV reflects your underlying health. It doesn't add to it. If you're sleeping well, exercising regularly, managing stress, and not drinking too much — your HRV is probably fine whether you look at it or not. Living well and never checking your HRV is a perfectly good strategy.
Where tracking has value is as a feedback tool. If you're making changes to your lifestyle and want to see whether they're registering physiologically, a gently improving HRV trend over weeks or months can be genuinely motivating. Some people find that useful. Others find it one more thing to worry about.
Personally, I don't track mine routinely. It won't factor into my emergency department practice. A passing glance now and again is enough for me.
But if you choose to track it, a few principles:
Follow weekly or monthly trends, not day-to-day changes. Daily swings of 10-15% are normal and not worth reacting to. Measure consistently — most wearables record overnight automatically, which gives the most stable readings. Don't compare to others — genetics and device error make cross-person comparison unreliable. What you're looking for is a stable baseline, or a gently improving one alongside positive lifestyle changes.
When to See Your Doctor
Most HRV variation is harmless. But certain patterns are worth acting on.
A sustained drop you can't explain. If your weekly average falls well below your normal range and stays there for more than a week — and you can't attribute it to poor sleep, stress, alcohol, or overtraining — speak to your doctor. This kind of shift can sometimes reflect the onset of illness before obvious symptoms appear. Research during the pandemic found wearable devices detected HRV changes up to seven days before a positive COVID test. This isn't unique to COVID — your HRV dips whenever your immune system activates, or when an underlying condition is developing.
If that sustained drop comes with symptoms — unexplained fatigue, exercise intolerance, palpitations, dizziness — that strengthens the case for investigation. A blood test can rule out common causes like thyroid dysfunction, anaemia, or metabolic changes.
Unusually high readings that coincide with feeling unwell. Research from the UK Biobank found a U-shaped relationship between HRV and mortality — very low and very high were both associated with increased risk. Extremely high HRV can indicate ectopic heartbeats or abnormal heart rhythms. If your readings spike well above your usual baseline and you feel unwell — particularly with palpitations or lightheadedness — that's worth investigating.
Any existing health condition that affects your heart or metabolism — cardiovascular disease, diabetes, hypertension — can influence your HRV readings. If you have a known condition, tracking HRV may have value, but discuss the readings with your doctor rather than interpreting them yourself. The context matters.
The Bottom Line
HRV is an interesting metric. It reflects real physiology and it correlates with meaningful health outcomes. But its clinical relevance for most people is still limited.
What isn't limited is the evidence behind the things that improve it: regular exercise, consistent sleep, moderate alcohol intake, and slow breathing. These matter whether your HRV is 25 or 75, and whether you ever look at the number or not.
If tracking motivates you, track it. If not, close the app and go for a walk. Invest your time and energy into living well. That's what actually matters.

Ready to Transform Your Health?
Get the complete Vital 3 Method guide — free:
Your HRV reflects your sleep, exercise, and nutrition. Get all three right and the number takes care of itself. My HRV improved from 60-74 using this exact framework.
Get the complete Vital 3 Method guide — free:
- The 3 highest-impact changes for each pillar (9 total)
- The Build Good Habits framework to make them stick
- Start with one, build from there — no overhaul required
No spam. Unsubscribe anytime.
Frequently Asked Questions
Sources
- Laborde S et al. (2022). Effects of voluntary slow breathing on heart rate and heart rate variability: A systematic review and a meta-analysis. Neuroscience & Biobehavioral Reviews. PubMed
- Amekran Y & El hangouche AJ (2024). Effects of Exercise Training on Heart Rate Variability in Healthy Adults: A Systematic Review and Meta-analysis. Cureus. PubMed
- Spaak J et al. (2010). Dose-related effects of red wine and alcohol on heart rate variability. American Journal of Physiology. PubMed
- Dial MB et al. (2025). Validation of nocturnal resting heart rate and heart rate variability in consumer wearables. Physiological Reports. PubMed
- O'Grady B et al. (2024). The Validity of Apple Watch for Serial Measurements of Heart Rate Variability. Sensors. PubMed
- Hirten RP et al. (2021). Use of Physiological Data From a Wearable Device to Identify SARS-CoV-2 Infection. JMIR. PubMed
- Brown L et al. (2021). The Effects of Mindfulness and Meditation on Vagally-Mediated Heart Rate Variability: A Meta-Analysis. Psychosomatic Medicine. PubMed
- Sjoberg NJ et al. (2011). Moderate weight loss improves heart rate variability in overweight and obese adults with type 2 diabetes. Journal of Applied Physiology. PubMed
Medical disclaimer
This content is for informational purposes only and is not intended as medical advice. Always consult your healthcare provider before making changes to your health routine. What works for one person may not work for another — this is a roadmap, not a prescription.
About Dr. Eoghan Colgan
Emergency medicine physician researching what actually works for longevity. I interview world-class experts in health and longevity and test everything personally. Everything I teach is what I'm implementing myself. More about me →

Related Articles
What Is Cardiometabolic Health? (And Why Only 7% of Us Pass)
What Is Cardiometabolic Health? (And Why Only 7% Pass) Key Takeaways It’s one system, not […]
What Is a Good Resting Heart Rate? (And Why “Normal” Isn’t the Same as Healthy)
What Is a Good Resting Heart Rate? (And Why “Normal” Isn’t the Same as Healthy) […]
Foods That Fight Fatigue: What Actually Works (And What Doesn’t)
Foods That Fight Fatigue: What Actually Works (And What Doesn’t) Key Takeaways It’s your eating […]



